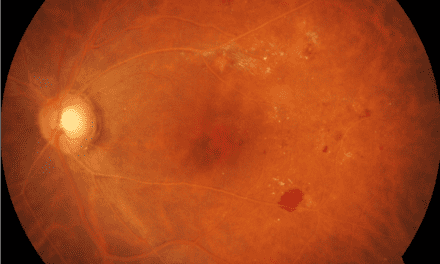
Subjective Dyschromatopsia as presenting symptom of Neovascular Age-Related Macular Degeneration

Abstract
Background: Subretinal fluid (SRF) is a possible finding associated with neovascular Age-related Macular Degeneration (AMD). SRF has been implicated as a cause of dyschromatopsia in other retinal conditions, such as Central Serous Chorioretinopathy (CSC), but not commonly in AMD. We report a case of sudden onset subjective dyschromatopsia associated with newly noted subretinal fluid secondary to neovascular AMD.
Case report: A 74-year-old Caucasian male presented to our clinic complaining of sudden onset color vision changes to the central vision of his left eye for approximately three days. His right eye’s vision was historically reduced due to a previous non-arteritic anterior ischemic optic neuropathy (NA-AION). He noted that distant objects, such as white or silver colored cars, appeared to be “mint green” in color until they were closer to him. The patient was diagnosed with neovascular AMD with associated SRF and referred to a retina specialist for treatment with anti-vascular endothelial growth factor (anti-VEGF) injections. The anti-VEGF treatment resolved the patient’s SRF and subjective dyschromatopsia, suggesting that the presence of SRF contributed to the dyschromatopsia.
Conclusion: Dyschromatopsia is a well-described phenomenon associated with chronic dry AMD, but it rarely will acutely cause a patient to note color vision disturbances. SRF has been implicated in other macular diseases, such as CSC, as a cause of acute dyschromatopsia. Dyschromatopsia may be related to photoreceptor displacement and the Stiles-Crawford Effect. We hypothesize that the patient’s monocular status and sudden onset of SRF due to neovascular AMD caused him to be acutely aware of his subjective dyschromatopsia, which directed him to seek treatment urgently.
Keywords: Age-related Macular Degeneration, Dyschromatopsia, OCT, OCTA, Stiles-Crawford Effect
Introduction
Age-related Macular Degeneration (AMD) is a leading cause of blindness in the United States, affecting approximately 20 million people.1 The Age-Related Eye Disease Study (AREDS) study classified AMD into four categories.2
-
- Category 1: The AREDS control group consisted of patients with no or few small drusen (< 63 microns in diameter).
- Category 2: Characterized by a combination of multiple small drusen, a few intermediate drusen (> 63 microns and < 124 microns in diameter or Retinal Pigment Epithelium (RPE) abnormalities such as pigment mottling.
- Category 3: Characterized by extensive intermediate drusen, at least one large druse (> 125 microns in diameter), or foveal-sparing geographic atrophy.
- Category 4: advanced/late AMD is characterized by one or more of the following findings: Geographic atrophy involving the fovea, choroidal neovascularization (CNV), serous or hemorrhagic detachment of the sensory retina or RPE, and disciform scarring.
In recent years there has been an updated consensus on the nomenclature for dictating findings related to AMD and, specifically, neovascular AMD.3 The terminology historically used in the literature is based on fluorescein angiography and does not apply to many features noted by newer imaging modalities such as Optical Coherence Tomography (OCT) and Optical Coherence Tomography Angiography (OCTA). For example, older terms such as Occult CNV and Classic CNV are now referred to as Type 1 Macular Neovascularization (MNV) and Type 2 MNV, respectively. Additionally, Neovascularization has been identified to originate from other areas than solely the choroid. Therefore, subclassification using OCT and OCTA to identify these features is becoming more widely accepted.
Neovascular AMD causes vision loss, central scotomas, and other less-reported visual dysfunctions. Due to the severity of visual dysfunction in the advanced stages of AMD, patients and doctors must monitor for signs and symptoms that may indicate the presence of neovascularization. Treatment is targeted against the release of vascular endothelial growth factor (VEGF) via anti-VEGF intravitreal injections.
Degenerative retinal diseases, such as AMD and other maculopathies, such as Central Serous Chorioretinopathy (CSC), can alter the cellular structure of the retina. This alteration can cause visual dysfunction of varying degrees, as measured by visual acuity, contrast sensitivity, color vision, and central visual field testing.4 Genetic factors, oxidative stress, and aging play a prominent role in the etiology of AMD. Chronic cigarette smoking is the most significant social risk factor for disease progression.
Like AMD, CSC also causes serous detachment of the sensory retina and retinal pigment epithelium (RPE) and may rank fourth in the incidence of non-surgical retinopathies after AMD, diabetic retinopathy, and branch retinal vein occlusion. CSC may be second only to AMD as the presumed cause of subretinal neovascularization.5 The cause of the serous detachment in CSC is not wholly understood; however, it has been correlated with choroidal thickening. Cheung et al. found the average choroidal thickness in controls to be 191-350 microns, whereas, in patients with CSC, choroidal thickness was 345-505 microns.6 Symptoms of acute CSC include blurred vision with relative central scotoma, metamorphopsia, dyschromatopsia, micropsia, and reduced contrast sensitivity. Dyschromatopsia in CSC is most often with a tritan axis7 and is thought to be associated with photoreceptor displacement and the Stiles-Crawford effect.8
It is reasonable to suspect that subretinal fluid, regardless of the underlying etiology, can cause visual disturbances, such as subjective dyschromatopsia. We discuss a case of AMD with sudden onset subjective dyschromatopsia due to subretinal fluid.
Case Report
No identifiable health information was included in this case report. A 74-year-old Caucasian male presented for a problem-focused examination after a five-year absence from our clinic. He complained of a several-day history of mildly reduced vision and changes to his color perception in the left eye. Specifically, he noted that lightly colored distant objects, such as cars, appeared “mint green” to him, but when the object got nearer, it appeared to be white or silver. His ocular history was remarkable for a previous non-arteritic anterior ischemic optic neuropathy in his right eye with subsequent reduced best-corrected visual acuity. He had a history of Type 2 diabetes mellitus without retinopathy or macular edema in either eye, early-stage nonexudative age-related macular degeneration bilaterally, and pseudophakia bilaterally. His systemic health was remarkable for type 2 diabetes mellitus, atrial fibrillation, hypothyroidism, obstructive sleep apnea, hypertension, asthma, and major depressive disorder.
Best corrected visual acuity was 20/800 in the right eye and 20/20-2 in the left eye. Color vision testing by Ishihara plates was unable to be completed due to reduced visual acuity in the right eye. The left eye missed plates #8 and #10, which was still considered a passing result. Extraocular motilities were noted to be smooth and full bilaterally. Confrontation fields were constricted inferonasally in the right eye and full to finger counting in the left eye. Pupils were equal, round, and reactive to light, with a longstanding right afferent pupillary defect attributed to his previous non-arteritic anterior ischemic optic neuropathy.Slit-lamp examination of the anterior segment was unremarkable. By applanation, intraocular pressure (IOP) was 13 mm/Hg in the right eye and 13 mm/Hg in the left eye at 2:28 PM. A dilated fundus examination revealed an approximate cup-to-disc ratio of 0.1 in each eye. The right optic nerve head was diffusely pale, while the left was pink and well-perfused. The right macula was flat with small to intermediate drusen and mild pigment clumping superior to the macula without evidence of subretinal fluid or hemorrhage. The left macula was also noted to have scattered small and intermediate drusen in addition to a large clinically detectable central elevation with the appearance of a pigment epithelial detachment (PED). No intraretinal or subretinal hemorrhaging was noted. Vessels and periphery were unremarkable, and the vitreous was clear in both eyes.
Updated optical coherence tomography (OCT) testing was obtained. The RNFL OCT showed diffuse total RNFL thinning in the right eye, consistent with the patient’s optic atrophy. The left eye’s RNFL OCT was unremarkable. The right eye’s macular OCT revealed a normal foveal contour with several extra-foveal sub-RPE hyperreflective elevations, consistent with the clinical appearance of intermediate drusen (Fig. 1A). There was no intraretinal or subretinal fluid noted. The left eye’s macular cube OCT demonstrated loss of the typical foveal contour due to a localized area of central subretinal fluid (Fig. 1B). Shallow irregular RPE elevation (SIRE) with adjacent subretinal fluid extended superior from the fovea. Six-by-six-millimeter OCT Angiography (OCTA) was also performed.

Figure 1. (A) Macular OCT B-scan image from patient’s right eye upon initial presentation. White arrows highlight presence of small to intermediate retinal drusen. (B) Macular OCT B-scan image from patient’s left eye upon initial presentation. Asterisk highlights area of the patient’s central subretinal fluid believed to be responsible for the patient’s subjective dyschromatopsia. OCT = Optical Coherence Tomography.
There were no areas concerning for MNV in the right eye. OCTA of the left eye demonstrated increased signal reflectivity on the RPE-RPE fit Angioplex analysis that was concerning for an area of Type 1 MNV. This area was located superotemporally to the fovea, which corresponded to the area of SIRE noted on the macular OCT cube (Figs. 2 and 3).

Figure 2. Three representative slices from the patient’s OCT-A of the left eye upon presentation. (A) Horizontal slice located superior to the fovea (blue horizontal line) demonstrates shallow irregular RPE elevation with choroidal flow (green) concerning for Type 1 MNV. (B) Horizontal slice located closer to the macula than (A) that again demonstrates RPE elevation with associated choroidal flow. (C) Slice located just superior to the foveal pit. A black area of fluid can be observed above the RPE but below the sensory retina, representing subretinal fluid likely originating from the suspected MNV located in slices (A) and (B). OCT-A = Optical Coherence Tomography Angiography. MNV = Macular Neovascularization. RPE = Retinal Pigment Epithelium.

Figure 3. En Face analysis of patient’s left OCT-A. (A) AngioPlex analysis of RPE-RPE-Fit slab reveals hyper-reflective area representative of suspected Type 1 MNV located supero-temporal to the fovea. (B) Structure analysis reveals significant structural irregularity within RPE-RPE-Fit slab. (C) Horizontal slice through hyperreflective area present on AngioPlex Analysis. Asterisk denotes SIRE corresponding with area of suspected Type 1 MNV. OCT-A = Optical Coherence Tomography Angiography. RPE = Retinal Pigment Epithelium. MNV = Macular neovascularization.
The patient was diagnosed as having intermediate nonexudative age-related macular degeneration in the right eye and active neovascular age-related macular degeneration in his left eye. He was started on AREDS 2 multivitamin supplementation and was referred to a retina specialist for evaluation and treatment.
Approximately two weeks later, the retina specialist evaluated the patient, confirmed diagnosis, and recommend treatment with intravitreal bevacizumab injections. Risks, benefits, and alternative treatments were discussed with the patient, who elected to proceed with a series of three intravitreal injections of bevacizumab, spaced approximately one month apart, in the left eye. The first injection was administered at that visit. When the patient returned to the retina specialist one month later for his second intravitreal injection, he noted subjective improvement in his left eye’s vision. He also noted the resolution of his dyschromatopsia. Entering acuity was measured to be stable at 20/30 in the left eye. Macular OCT revealed resolution of subretinal fluid and restoration of a normal foveal contour. Macular change analysis showed a 47-um reduction in central macular subfield thickness compared to the date of initial treatment (Fig. 4). The area of SIRE superior to the fovea remained stable in appearance. The patient was instructed to continue his AREDS 2 vitamin supplementation and again follow up in one month.

Figure 4. Timeline of left eye’s macular OCT and ETDRS thickness grid. Day zero represents the patient’s initial presentation to our eye clinic. Day 14 was the first time the retina specialist examined and treated the patient with intravitreal bevacizumab. Day 59 was the patient’s 1-month follow-up and second intravitreal injection of bevacizumab. Day 87 was the patient’s subsequent monthly follow-up and final injection of the initial treat and extend protocol. Central subretinal fluid was present on days zero and 14 but absent following intravitreal injection of bevacizumab on day 14. Central ETDRS subfield thickness was reduced by approximately 40-50 um following the initiation of treatment. The patient’s subjective dyschromatopsia resolved once the subretinal fluid was no longer detectable by OCT. OCT = Optical Coherence Tomography. EDTRS = Early Treatment of Diabetic Retinopathy Study.
Approximately four weeks later, the patient returned to the retina specialist for his final intravitreal injection of the series, still noting that his vision remained good and that he continued not to notice dyschromatopsia. Objectively his acuity was slightly reduced to 20/40 in the left eye. Macular OCT revealed stable findings without central subretinal fluid. Following this visit, the patient continued care with the retina specialist on a treat and extend basis, with no mention of the return of his dyschromatopsia.
Discussion
The diagnostic criteria historically crucial to evaluating a patient’s AMD are well known. Visual acuity, metamorphopsia, dyschromatopsia, and a central scotoma with worsening symptoms over time are characteristic of progressive AMD. A 2012 study of treatment requiring AMD highlighted symptoms with a higher predictive value regarding the need for treatment. Among those symptoms is dyschromatopsia.9
Normal color vision is generated by comparing short, medium, and long wavelengths by cone photopigment cells. Short wavelength cone signals give perceived blue-yellow channels, while medium and long cone signals give red-green channels.10 Changes to the perception of color in the setting of macular degeneration are frequently described in the literature and generally progress slowly over time. As such, it is not a typical symptom that would acutely alert a patient to seek care, as it did in this case.
In the 1920s, during a time of increasing traffic light prevalence, a government physicist named W. Stanley Stiles was assigned to investigate street lighting related to visibility and glare.11 Eventually, he derived an equation to quantify these features as a variable of pupil size: the larger the pupil, the brighter a given object should appear. However, Stiles and his colleague, B.H. Crawford later discovered this was only sometimes the case. Equal light rays entering the eye through different points of the pupil produce a visual impression differing in brightness and color even though the same point of the retina, such as the fovea, is stimulated. This is now recognized as the Stiles-Crawford effect.
This case exemplifies an approach to the Stiles-Crawford effect not frequently considered. Rather than the orientation of the entering light rays resulting in a change in luminous efficiency, photoreceptor orientation plays a role due to mechanical disturbances within the retina. Dyschromatopsia, in this case, likely arises from subretinal fluid displacing the central photoreceptors. This phenomenon was first described by Stiles in the 1930s and is known as directional sensitivity: light rays entering the eye through different points of the pupil and terminating on the same point of the retina are incident on the retina in different directions and result in variations in visual response.12
One must then consider the anatomical differences between rods and cones and why this phenomenon is most prominent in photopic vision. In healthy eyes, the foveal cone photoreceptors point toward the center of the pupil. As a result, more light is reflected towards the center of the pupil than towards the pupil edges.
Much like subretinal fluid seen in exudative AMD, CSC can present as a localized sensory retinal detachment caused by serous fluid. In a study involving a 35-year-old woman with CSC, a foveal reflection analyzer (FRA) was used to measure the optical Stiles-Crawford effect. The FRA showed that the presence of subretinal fluid caused disorientation of the foveal cone-photoreceptors and that it took a surprisingly long time after the subretinal fluid had disappeared for the foveal cones to regain their normal orientation. In this case, it took 56 weeks after onset for recovery to be within normal limits.8 While this patient initially presented due to the onset of a small central scotoma, it has been noted elsewhere that at the time of active CSC or accumulation of subretinal fluid, a blue-yellow color vision defect is common.13
In either circumstance of sensory retinal detachment, a comparison of OCT images regarding outer retinal structure shows progressive thinning because of tissue loss when a detachment persists. Serous detachment separates the photoreceptors from the retinal pigment epithelium and the choriocapillaris, separating them from their source of oxygen and nutrients resulting in photoreceptor death. Changes seen early on in this separation include disorganization, fragmentation, and dismantling of the outer segment disks. Still, it has been challenging to quantify the exact time frame between separation and photoreceptor death as studies have shown variation between 50 days and more than one year. It is believed that the high concentration of nourishment in the subretinal fluid connected with the tissue fluid in the choroid provides oxygen and glucose, which prolongs photoreceptors’ integrity.14
The degree of preservation of the outer plexiform layer (OPL) directly correlates with the degree of visual acuity loss. The same can be inferred for color vision changes, which depend on the duration of detachment. In this case, subretinal fluid was identified and treated within 14 days of presentation. Quick identification, treatment, and resolution led to a better visual outcome and complete resolution of color vision changes by day 59, where subretinal fluid was completely absent.
The same study that evaluated visual acuity noted that the OPL after serous detachment was always thicker and distorted at the fovea. This suggests subfoveal serous retinal detachments have a more significant impact on cones than rods and, in turn, on color vision.14 A different study by Maaranen et al. supported this finding. Also, it noted the lack of correlation between the onset of serous detachment and color vision changes suggesting that the subretinal fluid seen in this case was the etiology for the acute onset of symptoms.13 While the recovery of color vision in eyes with serous detachments cannot yet be predicted, it has been shown to linger for many years after active disease. This was shown by examining color vision using the Standard Pseudoisochromatic Plates Part 2 (SPP2), FM-100 and Spectrum Color Vision Meter 712 anomaloscope, which showed abnormal scores for up to 19 years following resolution of active disease. Our patient displayed complete resolution of subjective color vision changes following the resolution of subretinal fluid; however, more specific objective color vision testing may have yielded different results. Ishihara color vision testing performed on our patient is meant to identify red-green color deficiencies and may not capture the blue-yellow deficiencies typically associated with these retinal conditions.
This case highlights the similarities of such a finding between two common etiologies of subretinal fluid in ocular disease. To differentiate the two, one may consider the presence or absence of micropsia. The development of this symptom requires a fovea-centered elevation but preserved central retinal function, as seen in CSC. The lack of micropsia was then noted to be an independent predictor for the presence of treatment-requiring exudative AMD.9
In addition to subretinal fluid, other retinal disruptions such as MNV may produce similar symptoms. As previously touched upon, there has been a recent shift in nomenclature regarding neovascular AMD based upon OCT and OCTA findings, rather than fluorescein angiography findings.3 Previously used terms such as occult CNV, classic CNV and retinal angiomatous proliferation have been replaced as Type 1, Type 2, and Type 3 MNV, respectively.
-
- Type 1 MNV is charactered by findings such as RPE elevation and vessels below the RPE on OCTA.
- Type 2 MNV demonstrates a vascular network located in the subretinal space.
- Type 3 MNV suggests intraretinal neovascularization that may grow toward the choroid.
Upon presentation, the patient’s OCTA demonstrated sub-RPE elevation with choroidal flow that was concerning for Type 1 MNV. A 2019 study looked to determine whether there are differences in visual outcomes between different types of neovascularization and found that eyes with occult CNV (or Type 1 MNV) had overall better visual acuity than other types at baseline and five years after being treated.15 Our patient’s visual acuity always remained 20/40 or better throughout his diagnosis and treatment, similar with the findings from this study.
Conclusion
While consideration must be made for all other physical transmission defects in the eye media and retina, this case represents a clinical course not-frequently documented in the literature. Acute onset of subjective color vision defects secondary to subretinal fluid with subsequent resolution following reabsorption is often associated with CSC but should also be considered in the setting of neovascular age-related macular degeneration.
REFERENCES
- Rein DB, Wittenborn JS, Burke-Conte Z, Gulia R, Robalik T, Ehrlich JR, et al. Prevalence of Age-Related Macular Degeneration in the US in 2019. JAMA Ophthalmol.2022;140(12):1202–1208. doi:10.1001/jamaophthalmol.2022.4401
- Age-Related Eye Disease Study Research Group. The Age-Related Eye Disease Study (AREDS): design implications. AREDS report no. 1. Control Clin Trials. 1999 Dec;20(6):573-600. doi: 10.1016/s0197-2456(99)00031-8.
- Spaide RF, Jaffe GJ, Sarraf D, Freund KB, Sadda SR, Staurenghi G,et al. Consensus Nomenclature for Reporting Neovascular Age-Related Macular Degeneration Data: Consensus on Neovascular Age-Related Macular Degeneration Nomenclature Study Group. Ophthalmology. 2020 May;127(5):616-636. doi: 10.1016/j.ophtha.2019.11.004. Epub 2019 Nov 14. Erratum in: Ophthalmology. 2020 Oct;127(10):1434-1435. PMID: 31864668.
- Arden GB, Wolf JE. Colour vision testing as an aid to diagnosis and management of age related maculopathy. Br J Ophthalmol. 2004 Sep;88(9):1180-5. doi: 10.1136/bjo.2003.033480.
- Wang, M., Munch, I.C., Hasler, P.W., Prünte, C. and Larsen, M. (2008), Central serous chorioretinopathy. Acta Ophthalmologica, 86: 126-145. https://doi.org/10.1111/j.1600-0420.2007.00889.x
- Cheung CMG, Lee WK, Koizumi H, Dansingani K, Lai TYY, Freund KB. Pachychoroid disease. Eye (Lond). 2019 Jan;33(1):14-33. doi: 10.1038/s41433-018-0158-4. Epub 2018 Jul 11.
- Williams CM. Visual acuity and colour vision tests–a preliminary report. Br J Physiol Opt. 1976;31(4):29-31. PMID: 1053022.
- Kanis MJ, van Norren D. Delayed recovery of the optical Stiles-Crawford effect in a case of central serous chorioretinopathy. Br J Ophthalmol. 2008;92(2):292-294. doi:10.1136/bjo.2007.120139
- Hessellund A, Larsen DA, Bek T. The predictive value of subjective symptoms and clinical signs for the presence of treatment-requiring exudative age-related macular degeneration. Acta Ophthalmologica. 2012;90(5):471-475. doi:10.1111/j.1755-3768.2010.02074.x
- Vemala R, Sivaprasad S, Barbur JL. Detection of Early Loss of Color Vision in Age-Related Macular Degeneration – With Emphasis on Drusen and Reticular Pseudodrusen. Investigative Ophthalmology & Visual Science. 2017;58(6):BIO247-BIO254. doi:10.1167/iovs.17-21771
- Westheimer G. Directional sensitivity of the retina: 75 years of Stiles–Crawford effect. Proc Biol Sci. 2008;275(1653):2777-2786. doi:10.1098/rspb.2008.0712
- Stiles WS. The directional sensitivity of the retina and the spectral sensitivities of the rods and cones. Proc R Soc Lond B. 127:64-105. doi:10.1098/rspb.1939.0012
- Maaranen TH, Tuppurainen KT, Mäntyjärvi MI. Color vision defects after central serous chorioretinopathy. Retina. 2000;20(6):633-637. doi:10.1097/00006982-200011000-00008
- Piccolino FC, de la Longrais RR, Ravera G, et al. The foveal photoreceptor layer and visual acuity loss in central serous chorioretinopathy. Am J Ophthalmol. 2005;139(1):87-99. doi:10.1016/j.ajo.2004.08.037
- Invernizzi A, Nguyen V, Teo K, et al. Five-Year Real-World Outcomes of Occult and Classic Choroidal Neovascularization: Data From the Fight Retinal Blindness! Project. American Journal of Ophthalmology. 2019;204:105-112. doi:10.1016/j.ajo.2019.03.001